The scar is a biological process of wound healing in the skin and other tissues of the body. A normal scar matures or remodels over 12-18 months, resulting in a final scar that has a tensile strength of 70-80% of uninjured skin. The amount of scarring may be determined by the wound size, location and depth, degree of wound contamination, person’s age, heredity, skin characteristics including skin colour and techniques of wound closure. Patients who present with unfavourable scars typically have wounds that:
- Demonstrate an unfavourable configuration with respect to length and direction of RSTLs (relax skin tension lines)
- Have undergone pathologic healing processes
- Situated in unfavourably cross anatomic regions
- Are subjected to constant deforming contractile forces because of underlying anatomy especially at the area of excessive movements or joint areas
- Are deeply traumatic
Types of unfavourable scars:
- Hypertrophy scar – occurs when the body produces collagen excessively, causing the scar to rise above the surrounding skin.
- Keloid – is a severe form of scarring because the scar may progressively overgrow the original wound margins to involve adjacent tissue.
- Atrophy scar – takes the form of a sunken recess in the skin, which has a pitted appearance due to loss of underlying structures supporting the skin, such as fat or muscle.
-
Stretch marks – are caused when the skin is stretched rapidly (during pregnancy, significant weight gain or adolescent growth spurts) or when skin is put under tension during the healing process, (usually near joints).
Scar revision consists of a spectrum of surgical techniques and other modalities aimed to reduce or improve the appearance of scars and restores function caused by an injury, wound, or previous surgery.
The timing of scar revision depends on a variety of factors, including type and location of the injury and the psychological readiness of the patient. One popular practice adopts a 6 to 12-month waiting period following the initial injury, but experience shows that this waiting period must be individualised because an earlier approach may be undertaken.
Treatment options for unfavourable scars may vary depending on the type and degree of scarring. They can be classified into:
- Simple topical treatments and pressure therapy – topical ointments (silicone), pressure garment.
- Minimally invasive procedures – chemical peels, dermabrasion, laser, steroid injections, filler or fat graft injections.
- Surgical revision procedures – ranging from simple scar excision to advanced techniques (tissue expansion or flap reconstruction) in wound closure.
It is essential to understand that a scar cannot be completely erased. The scar revision procedure is meant to minimise the scar so that it is more consistent with the surrounding skin tone and texture. Thus, providing a more pleasing cosmetic result or improve a scar that has healed poorly.
Case No. 1:
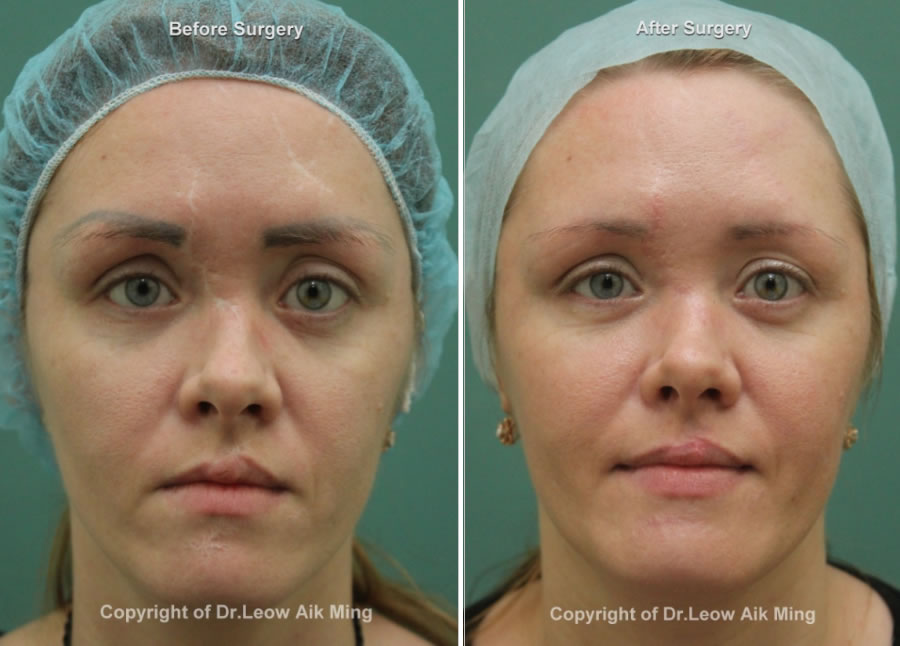
Case No. 2:
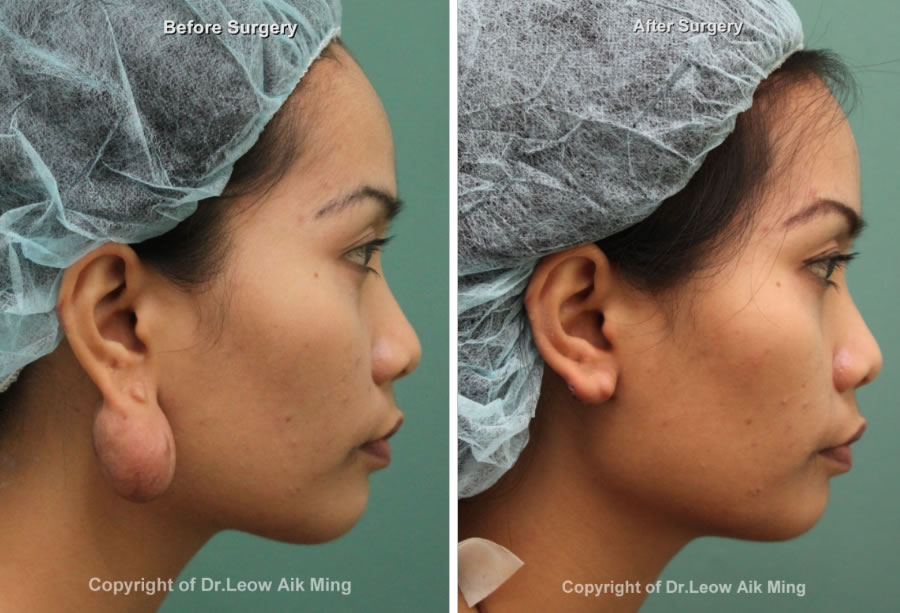
Case No. 3:
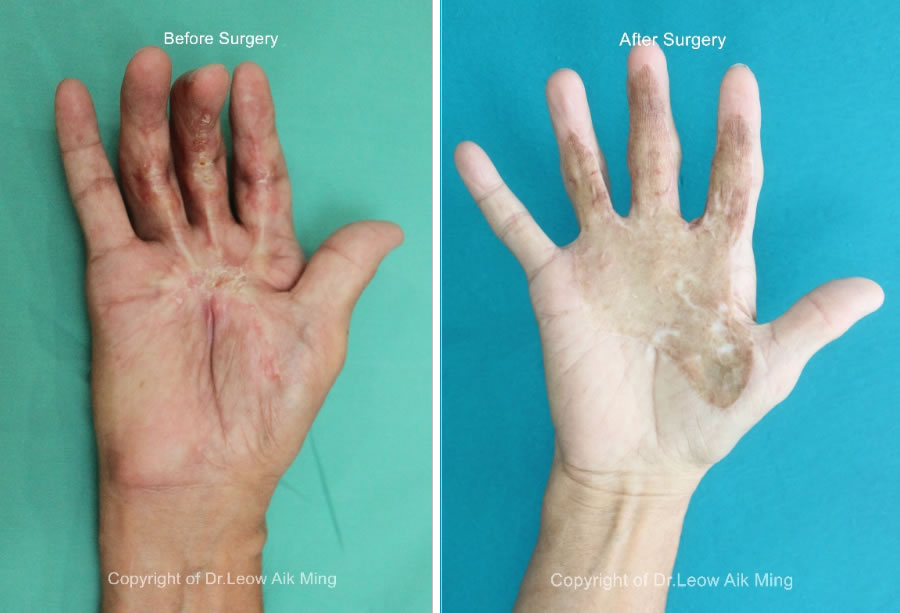
Ideal candidates for scar revision
- Patients who are bothered by scars anywhere on the face or body
- Individuals with a positive outlook and realistic expectations
- Do not have active skin infection/inflammation (such as active acne) or other skin diseases in the area to be treated
- Healthy individuals who do not have medical conditions that can impair healing or increase the risk of surgery
Preoperative evaluation for scar revision
Communication is vital to achieving the patient’s goals. During the initial consultation, patients will have the opportunity to discuss their goals and desired results with the plastic surgeon. The plastic surgeon will work closely with the patients to reach an agreement about the expectations from the surgical procedures involved and their long term benefits. Every patient is different. Therefore, a specific treatment regimen is planned to suit an individual’s need. The preoperative evaluation for scar revision includes:
- Discussion about reasons for corrective surgery, patients’ expectations and desired outcome
- >Medical conditions, drug allergies and previous medical or surgical treatment
- Use of current medications, vitamins, herbal supplements, alcohol, tobacco and drugs
- Discussion on anaesthesia and its risks
- Physical examination
- Scar examination including detailed assessments of their size and shape and surrounding skin quality
- Photography for preoperative and postoperative evaluation
Preparation for scar revision
- Get laboratory testing or a medical evaluation
- Evaluation of general health status and any pre-existing health conditions or risk factors
- Adjust medications if for specific medical conditions
- Stop smoking and alcohol well in advance of the scheduled date for surgery
- Avoid taking aspirin, anti-inflammatory drugs and herbal supplements before surgery
- Special instructions will be given on the day before and after surgery
The risks and safety information on scar revision
The decision to have scar revision surgery is extremely personal. Patients have to consider if the benefits will achieve their goals, and if the risks and potential complications are acceptable. Therefore, it is crucial for patients to understand that every surgical procedure has its complications and downtime. However, if a patient is appropriately assessed before the surgery and postoperative care is given adequately, these risks can be eliminated or reduced.
Some of the common risks of scar revision surgery:
- Infection
- Bleeding
- Poor wound healing
- Wound breakdown
- >Skin discolouration
- Skin contour irregularities
- Skin sensitivity
- Swelling due to a blood clot or fluid accumulation
- Injury to deeper structures such as nerves, blood vessels or muscles
- Implant failure or infection (if implant such as tissue expander is used)
- Possibility of revision or staged surgery
- Anaesthesia risks
Postoperative expectations
Postoperative expectations following scar revision procedures vary depending upon the invasiveness of the procedure. Minimal invasive procedures (chemical peels, dermabrasion, laser, steroid injections, filler or fat graft injections) or simple scar revision surgery can be done as an out-patient basis. These procedures have shorter recovery time, and patients may resume their routine activities with 3 -5 days after the procedures. On the other hand, scar revision surgery that requires insertion of a tissue expander or flap surgery may need a longer recovery period. The initial healing phase for scar revision surgery may include localised swelling, discolouration or discomfort and this may take 1 to 2 weeks. The healing process will continue for several weeks to months for the new scar to fully restore and fade. The final result of the scar revision surgery is usually long-lasting.
Postoperative care
- Regular application of prescribed ointment and cleaning the involved areas as instructed
- Avoid excessive sun exposure during the healing phase
- Daily use of moisturiser and sunscreen on the new scar area
- Application of topical scar gel and massage around the new scar area will improve the appearance and texture of the scar
How much will a scar revision surgery cost?
Cost is always a consideration in elective surgery. The cost of scar revision surgery can vary widely.
The cost of scar revision surgery may include:
- Surgeon’s fee
- Hospital or surgical facility costs
- Anaesthesia fees
- Medical tests
- Post-surgical garment (optional) and
- Prescriptions for medication
Most health insurance companies do not cover scar revision surgeries, related complications or another surgery to revise the appearance of your scar. Carefully review your policy or find out more from your medical insurance agent. Patients are advised to contact their insurance company for further verification well in advance of surgery.
